Blog
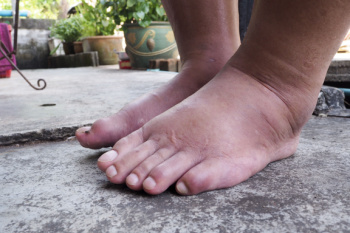
Diabetes affects the body in many ways, and one common issue is swollen feet. High blood sugar levels can damage blood vessels and nerves, leading to poor circulation and fluid retention in the lower extremities. This swelling, known as edema, can cause discomfort and may increase the risk of infections and ulcers. Nerve damage, or neuropathy, can further complicate the issue by reducing sensation, making it difficult to notice injuries or pressure points. Poor circulation slows healing, increasing the likelihood of complications. Managing blood sugar levels, wearing supportive footwear, and elevating the feet can help reduce swelling. If you have diabetes and your feet are noticeably swollen, it is suggested that you are under the care of a podiatrist who can help you to manage this condition.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Dean D. Hinners from Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

An ingrown toenail occurs when a toenail grows improperly into the surrounding skin, or when the skin around the nail grows too quickly, partially covering the nail. Ingrown toenails often result from improper nail trimming, such as cutting the nail into a curve instead of straight across, or wearing shoes that are too narrow and place excessive pressure on the toes. At first, an ingrown toenail may cause mild discomfort, but as it worsens, the area can become painful, red, and swollen, especially when pressure is applied. If left untreated, infection may develop, leading to pus formation and increased pain. A podiatrist can treat the toenail by gently lifting the edge of it and placing sterile cotton or a flexible tube beneath it to relieve pressure. If the nail is deeply ingrown or infected, this foot doctor may numb the toe and remove the ingrown section to reduce inflammation and prevent recurrence. If you need help with a painful or infected ingrown toenail, it is suggested that you schedule an appointment with a podiatrist for an exam and appropriate treatment solutions.
Ingrown toenails may initially present themselves as a minor discomfort, but they may progress into an infection in the skin without proper treatment. For more information about ingrown toenails, contact Dr. Dean D. Hinners of Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails are caused when the corner or side of a toenail grows into the soft flesh surrounding it. They often result in redness, swelling, pain, and in some cases, infection. This condition typically affects the big toe and may recur if it is not treated properly.
Causes
- Improper toenail trimming
- Genetics
- Improper shoe fitting
- Injury from pedicures or nail picking
- Abnormal gait
- Poor hygiene
You are more likely to develop an ingrown toenail if you are obese, have diabetes, arthritis, or have any fungal infection in your nails. Additionally, people who have foot or toe deformities are at a higher risk of developing an ingrown toenail.
Symptoms
Some symptoms of ingrown toenails are redness, swelling, and pain. In rare cases, there may be a yellowish drainage coming from the nail.
Treatment
Ignoring an ingrown toenail can have serious complications. Infections of the nail border can progress to a deeper soft-tissue infection, which can then turn into a bone infection. You should always speak with your podiatrist if you suspect you have an ingrown toenail, especially if you have diabetes or poor circulation.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.

Cracked heels develop when the skin on the feet becomes dry and loses its elasticity, leading to painful fissures. One common cause is prolonged pressure on the feet from standing for long hours or wearing shoes with inadequate support. Dry skin, often worsened by cold weather or dehydration, makes the heels more prone to cracking. Athlete's foot, a fungal infection, can cause peeling and flaking that leads to skin breakdown. Conditions such as eczema and psoriasis contribute to excessive dryness and inflammation, further increasing the risk of heel fissures. Without proper care, cracks can deepen and cause discomfort or infection. If you notice the beginning symptoms of cracked heels, it is suggested that you promptly contact a podiatrist who can offer you effective relief and prevention tips.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Dr. Dean D. Hinners from Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.

