Blogs
Recognizing Athlete’s Foot
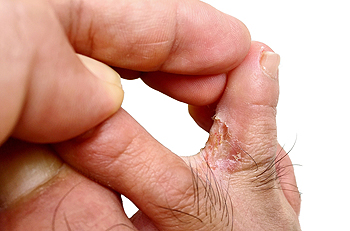
Athlete’s foot is a common fungal infection that affects the skin on the feet, particularly between the toes. Key signs include itching, burning, and redness, often accompanied by peeling or cracking skin. In more severe cases, blisters may develop, leading to further discomfort and possible secondary infections. The primary cause of athlete’s foot is the fungus known as trichophyton, which thrives in warm, damp environments, and tight-fitting shoes. Factors like excessive sweating, poor foot hygiene, and sharing personal items can increase the risk of infection. Understanding these signs and causes is essential for early identification and effective treatment. If you have symptoms of athlete’s foot, it is suggested that you consult a podiatrist who can offer you effective relief and treatment solutions.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with Dr. Dean D. Hinners from Illinois. Our doctor will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
- Thoroughly washing and drying feet
- Avoid going barefoot in locker rooms and public showers
- Using shower shoes in public showers
- Wearing socks that allow the feet to breathe
- Changing socks and shoes frequently if you sweat a lot
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
- Redness
- Burning
- Itching
- Scaly and peeling skin
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Why Do Children Have Flat Feet?

Flat feet, or fallen arches, are common in children and can be attributed to various factors. Genetic predisposition often plays a significant role, as flat feet can run in families. In many cases, children may develop arches as they grow, but some may continue to have flat feet into adulthood. Other contributing factors include ligament laxity and muscle weakness, which can affect the foot's structure. Symptoms of flat feet often include discomfort or pain in the feet, especially after prolonged activity. Children may also experience fatigue, difficulty standing for long periods, or balance issues. Flat feet can lead to complications such as pain in the knees, hips, or lower back. If your child is experiencing pain or discomfort from having flat feet, it is suggested that you contact a podiatrist who can provide effective relief solutions.
Flatfoot is a condition many people suffer from. If you have flat feet, contact Dr. Dean D. Hinners from Illinois. Our doctor will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
- Pain around the heel or arch area
- Trouble standing on the tip toe
- Swelling around the inside of the ankle
- Flat look to one or both feet
- Having your shoes feel uneven when worn
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
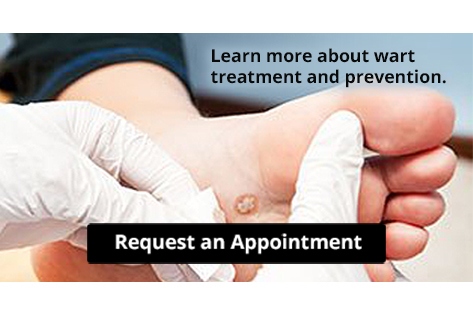
Plantar Warts Can Be Treated!
Protecting Your Toes When Hiking

Hiking can put significant stress on your toes, especially when going down steep trails. The repeated impact of your foot sliding forward and striking the front of your shoes can result in pain, blisters, and even bruised toenails. To protect your toes during hikes, it is important to wear properly fitted shoes that are ideally a half-size larger to allow for swelling. The so-called heel lock technique involves lacing shoes tightly around the ankle. This helps to keep the heel in place, thereby preventing the foot from sliding forward in your shoe. Maintaining well-trimmed toenails and using moisture-wicking socks can reduce friction and prevent blisters. Additionally, trekking poles can redistribute your body weight, which lessens the pressure on your toes, particularly during downhill hikes. If left untreated, toe pain from hiking may lead to more serious issues, including joint dysfunction or gait changes. If you experience toe pain after hiking, it is suggested that you schedule an appointment with a podiatrist for treatment.
Toe pain can disrupt your daily activities. If you have any concerns, contact Dr. Dean D. Hinners of Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Non-Surgical Treatment for Bunions
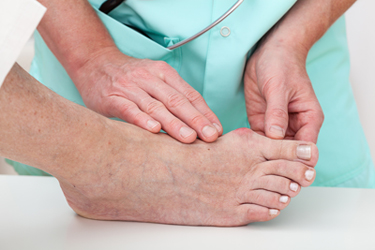
Bunions, a bony bump at the base of your big toe, can result from a misalignment of bones and tissues that pushes the toe inward. While surgery is the only way to completely remove a bunion, nonsurgical bunion treatments can effectively manage symptoms and slow progression. Wearing shoes with a wide toe box and low heels can reduce pressure on the bunion. Custom orthotics can help with proper foot alignment. Toe spacers and splints can also relieve discomfort by preventing further misalignment, although they will not permanently correct the bone structure. Stretching exercises may increase flexibility and ease pain, but they will not reverse the bunion itself. If your bunion is causing discomfort, consulting a podiatrist early can lead to treatment options that delay or prevent further complications. If you have pain caused by a bunion, it is suggested that you schedule an appointment with a podiatrist for guidance.
If you are suffering from bunions, contact Dr. Dean D. Hinners of Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What is PAD?
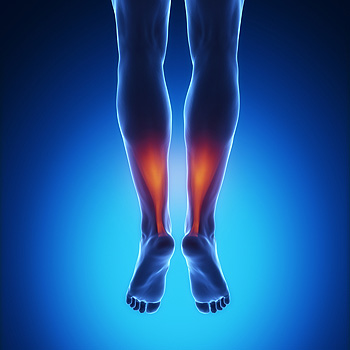 The medical term that is known as peripheral arterial disease (PAD) is described as excess fatty deposits in the arteries. This condition may inhibit blood supply to the feet, and it may be difficult to walk. Patients who are afflicted with PAD may experience a loss of feeling or a tingling sensation in the feet and legs, open sores which do not heal in a timely fashion, and the nails may become brittle. There are a variety of reasons why this condition may occur. These can consist of smoking, having elevated blood pressure, or being diabetic. Painful symptoms may be gradually diminished when gentle stretching techniques are frequently practiced, in addition to implementing healthy eating habits. If you are suffering from PAD, it is recommended that you consult with a podiatrist who can help you to manage this ailment.
The medical term that is known as peripheral arterial disease (PAD) is described as excess fatty deposits in the arteries. This condition may inhibit blood supply to the feet, and it may be difficult to walk. Patients who are afflicted with PAD may experience a loss of feeling or a tingling sensation in the feet and legs, open sores which do not heal in a timely fashion, and the nails may become brittle. There are a variety of reasons why this condition may occur. These can consist of smoking, having elevated blood pressure, or being diabetic. Painful symptoms may be gradually diminished when gentle stretching techniques are frequently practiced, in addition to implementing healthy eating habits. If you are suffering from PAD, it is recommended that you consult with a podiatrist who can help you to manage this ailment.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Dr. Dean D. Hinners from Illinois. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
An Overview of Clubfoot

Clubfoot is a congenital condition where a baby’s foot or feet are abnormally twisted. This deformity causes the foot to point downward and inward, resembling a club. It occurs due to an abnormal development of the tendons, muscles, and bones of the foot. The exact cause is often unclear but may involve genetic and environmental factors. Diagnosis typically occurs through physical examination shortly after birth, where the abnormal positioning is evident. In some cases, clubfoot affects both feet, known as bilateral clubfeet. Symptoms include an abnormal foot shape, limited movement, and difficulty placing the foot flat on the ground. If your child has clubfoot, it is strongly suggested that you contact a podiatrist who can properly diagnose the condition, and begin treatment which may include specific stretches, casting, or surgery to increase mobility.
Congenital foot problems require immediate attention to avoid future complications. If you have any concerns, contact Dr. Dean D. Hinners of Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
Congenital foot problems are deformities affecting the feet, toes, and/or ankles that children are born with. Some of these conditions have a genetic cause while others just happen. Some specific foot ailments that children may be born with include clubfeet, polydactyly/macrodactyly, and cleft foot. There are several other foot anomalies that can occur congenitally. What all of these conditions have in common is that a child may experience difficulty walking or performing everyday activities, as well as trouble finding footwear that fits their foot deformity. Some of these conditions are more serious than others. Consulting with a podiatrist as early as possible will help in properly diagnosing a child’s foot condition while getting the necessary treatment underway.
What are Causes of Congenital Foot Problem?
A congenital foot problem is one that happens to a child at birth. These conditions can be caused by a genetic predisposition, developmental or positional abnormalities during gestation, or with no known cause.
What are Symptoms of Congenital Foot Problems?
Symptoms vary by the congenital condition. Symptoms may consist of the following:
- Clubfoot, where tendons are shortened, bones are shaped differently, and the Achilles tendon is tight, causing the foot to point in and down. It is also possible for the soles of the feet to face each other.
- Polydactyly, which usually consists of a nubbin or small lump of tissue without a bone, a toe that is partially formed but has no joints, or an extra toe.
- Vertical talus, where the talus bone forms in the wrong position causing other bones in the foot to line up improperly, the front of the foot to point up, and the bottom of the foot to stiffen, with no arch, and to curve out.
- Tarsal coalition, when there is an abnormal connection of two or more bones in the foot leading to severe, rigid flatfoot.
- Cleft foot, where there are missing toes, a V-shaped cleft, and other anatomical differences.
- Macrodactyly, when the toes are abnormally large due to overgrowth of the underlying bone or soft tissue.
Treatment and Prevention
While there is nothing one can do to prevent congenital foot problems, raising awareness and receiving neonatal screenings are important. Early detection by taking your child to a podiatrist leads to the best outcome possible.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Plantar Fasciitis Relief

Plantar fasciitis is a common foot condition that causes pain in the heel and the bottom of the foot. It occurs when the plantar fascia, a thick band of tissue that runs along the bottom of your foot and connects the heel bone to the toes, becomes inflamed. This inflammation is often due to overuse, excessive pressure, or improper footwear. People with plantar fasciitis typically experience sharp, stabbing pain, especially in the morning or after long periods of rest. To manage plantar fasciitis, it is important to rest and avoid activities that can worsen the pain. Wearing supportive shoes can help to reduce strain. In more severe cases, corticosteroid injections, or even surgery may be necessary to achieve relief. If you have plantar fasciitis, it is strongly suggested that you schedule an appointment with a podiatrist for treatment.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Dean D. Hinners from Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Injuries From Pickleball on the Rise

As pickleball continues to rise in popularity, so does the incidence of foot injuries among players. This fast-paced sport, which combines elements of tennis, badminton, and ping-pong, involves quick lateral movements, sudden pivots, and constant pressure on the feet, making them vulnerable to various injuries. Common foot injuries in pickleball include plantar fasciitis, Achilles tendonitis, and stress fractures. These injuries are often the result of inadequate footwear, overuse, or insufficient warm-up and stretching before play. Players may also experience ankle sprains from sudden changes in direction, a frequent occurrence in the game. Preventing foot injuries in pickleball starts with wearing proper court shoes that offer good support and cushioning. Regular stretching exercises, particularly focusing on the calves and Achilles tendon, can also help. Additionally, gradually increasing play intensity and taking rest days can reduce the risk of overuse injuries. If you enjoy pickleball but have incurred a foot injury, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment.
Ankle and foot injuries are common among athletes and in many sports. They can be caused by several problems and may be potentially serious. If you are feeling pain or think you were injured in a sporting event or when exercising, consult with Dr. Dean D. Hinners from Illinois. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Common Injuries
The most common injuries that occur in sporting activities include:
- Achilles Tendonitis
- Achilles Tendon Rupture
- Ankle Sprains
- Broken Foot
- Plantar Fasciitis
- Stress Fractures
- Turf Toe
Symptoms
Symptoms vary depending upon the injury and in some cases, there may be no symptoms at all. However, in most cases, some form of symptom is experienced. Pain, aching, burning, bruising, tenderness, tightness or stiffness, sensation loss, difficulty moving, and swelling are the most common symptoms.
Treatment
Just as symptoms vary depending upon the injury, so do treatment options. A common treatment method is known as the RICE method. This method involves rest, applying ice, compression and elevating the afflicted foot or ankle. If the injury appears to be more serious, surgery might be required, such as arthroscopic or reconstructive surgery. Lastly, rehabilitation or therapy might be needed to gain full functionality in the afflicted area. Any discomfort experienced by an athlete must be evaluated by a licensed, reputable medical professional.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
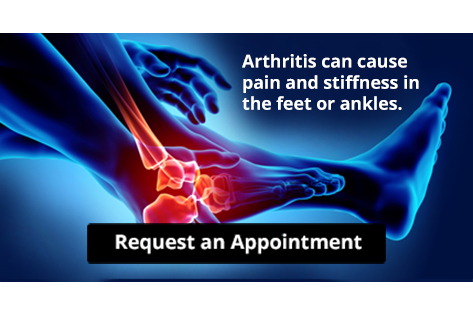
Arthritis Can Cause Pain in the Feet and Ankles
More...
Explaining Laser Treatment for Fungal Toenails
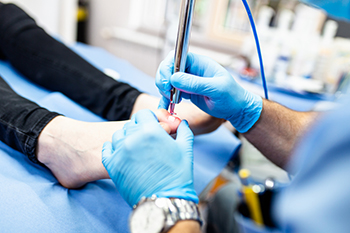
Laser treatment for fungal toenails is a modern approach that targets the infection with concentrated light, effectively reducing or eliminating the fungus. This procedure is particularly beneficial for individuals who may not tolerate oral antifungal medications, such as those with liver or kidney issues, diabetes, or older adults. During the procedure, a podiatrist uses a specialized device to shine light onto the affected nails, which may destroy or inhibit the growth of the fungus. This non-invasive treatment typically causes minimal discomfort, with most patients able to resume their regular activities immediately. Results of laser toenail treatment are not immediate and may take a couple of months to become noticeable, with full nail regrowth taking longer. Multiple sessions might be necessary to achieve the desired outcome. If you have fungal toenail problems, it is suggested that you schedule an appointment with a podiatrist to see if laser treatment is right for you.
Laser treatment can be an effective way to get rid of toenail fungus. If you have any questions about laser treatment, consult with Dr. Dean D. Hinners from Illinois. Our doctor will assess your condition and provide you with quality treatment for fungal nails.
What Are Toenail Fungal Infections?
Onychomycosis, or fungal infection of the nail, is a relatively common and non-serious condition. Around 10 percent of U.S. citizens are afflicted with fungal nails. Common forms of fungus that infect the nail include dermatophytes, yeasts, and molds.
Symptoms of Toenail Fungal Infections Include:
- Nail thickening
- Brittleness of the nail
- Discoloration of the nail
Diagnosis for Fungal Nails
Fungal infections are diagnosed by fungal culture and microscopy. This will rule out any other conditions such as nail trauma, psoriasis, lichen planus, and onychogryphosis.
What Is Laser Treatment?
Laser treatment is a non-invasive, safe, quick, and painless procedure that uses the heat from a laser to kill fungus in the nail. Each infected nail is targeted with a laser for several minutes. The treatment is usually utilized several different times over a select period. During this time, a podiatrist will keep an eye on the infection.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Heel Spur Information
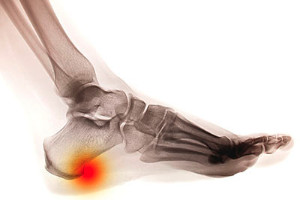
A heel spur is a bony growth that forms on the underside of the heel bone, often causing significant discomfort. This condition typically arises from repetitive stress or strain on the foot, which can lead to inflammation of the plantar fascia, the ligament that supports the arch. Risk factors can include obesity, prolonged standing, improper footwear, and activities that put excessive pressure on the feet. The main symptom is sharp, stabbing pain in the heel, particularly during the first steps in the morning or after periods of rest. To prevent heel spurs, it is essential to wear supportive shoes, maintain a healthy weight, and avoid excessive strain on the feet. Stretching exercises for the Achilles tendon and the plantar fascia can also help reduce the risk of developing this condition. If you have heel pain, it is suggested that you promptly schedule an appointment with a podiatrist who can accurately diagnose and treat heel spurs.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact Dr. Dean D. Hinners from Illinois. Our doctor will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the latest in diagnostic and treatment technology to meet your needs.
Negatives of Wearing Flip Flops

Flip-flops, while convenient and casual, are not ideal for foot health. Their lack of arch support and cushioning can lead to issues like foot pain, poor posture, and increased risk of injury. The minimal support may worsen conditions like plantar fasciitis and contribute to misalignment of the feet. Flip-flops also offer little protection from sharp objects or uneven surfaces, making them unsuitable for extended walking or physical activities. They are best worn for brief periods in low-risk environments, such as the poolside or beach, where minimal foot protection is needed. For daily wear or activities that involve prolonged standing or walking, opt for footwear that provides proper arch support and cushioning to promote overall foot health and comfort. Foot conditions may develop when flip flops are frequently worn. If this applies to you, it is suggested that you consult a podiatrist for treatment and who can guide you toward more appropriate shoe choices.
Flip-flops are not always the best choice of footwear. If you have any concerns about your feet or ankles, contact Dr. Dean D. Hinners from Illinois. Our doctor will assist you with all of your foot and ankle needs.
Flip-Flops and Feet
When the weather starts warming up, people enjoy wearing flip-flops. Flip-flops are comfortable, stylish, and easy to slip on and off; they're perfect for any summer beach goer. However, these shoes can cause harm to the feet.
How Can Flip-Flops Affect Me Long-Term?
- Ankle problems
- Hip problems
- Lower back problems
- Pain in the balls of the feet
- Problems with foot arches
- Changes in the way you walk
Are There Injuries Associated with Flip-Flops?
Yes. Since flip-flops are relatively weak and do not provide the same amount of support as sneakers, people who wear flip-flops regularly are more susceptible to injuries. On top of that, the open nature of the shoe makes your feet more prone to other problems, such as cuts and even infections. Common injuries and ailments include:
- Sprained ankles
- Blisters
- Infections
- Cuts and Scrapes
I like Wearing Flip-Flops. Are There Safe Alternatives?
When buying flip-flops, try to find ones that have sturdy soles and that are made of high-quality materials that will support for your feet. These flip-flops will cost more but will also last longer as a result.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Minimally Invasive Achilles Tendon Surgery
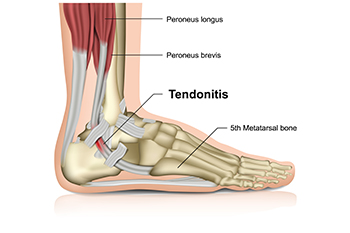 The Achilles tendon, the strongest tendon in the body, connects the calf muscles to the heel bone and is important for walking, running, and jumping. Achilles tendon injuries, such as ruptures, often result from sudden increases in activity or trauma. Conservative treatment for Achilles tendon injuries includes rest, compression, and elevation, in addition to immobilization with a cast or brace to allow natural healing. This approach is typically recommended for less severe injuries or for patients who may not be suitable candidates for surgery. Minimally invasive Achilles tendon repair surgery involves making small incisions to stitch the torn ends of the tendon together. This method reduces the risk of infection, minimizes scarring, and often leads to faster recovery times compared to traditional open surgery. Choosing between conservative treatment and surgery depends on the injury's severity, the patient’s activity level, and overall health. If you have injured your Achilles tendon, it is strongly suggested that you schedule an appointment with a podiatrist to help you determine the best course of treatment.
The Achilles tendon, the strongest tendon in the body, connects the calf muscles to the heel bone and is important for walking, running, and jumping. Achilles tendon injuries, such as ruptures, often result from sudden increases in activity or trauma. Conservative treatment for Achilles tendon injuries includes rest, compression, and elevation, in addition to immobilization with a cast or brace to allow natural healing. This approach is typically recommended for less severe injuries or for patients who may not be suitable candidates for surgery. Minimally invasive Achilles tendon repair surgery involves making small incisions to stitch the torn ends of the tendon together. This method reduces the risk of infection, minimizes scarring, and often leads to faster recovery times compared to traditional open surgery. Choosing between conservative treatment and surgery depends on the injury's severity, the patient’s activity level, and overall health. If you have injured your Achilles tendon, it is strongly suggested that you schedule an appointment with a podiatrist to help you determine the best course of treatment.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact Dr. Dean D. Hinners of Illinois. Our doctor will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
- Removing foot deformities like bunions and bone spurs
- Severe arthritis that has caused bone issues
- Cosmetic reconstruction
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
- Bunionectomy for painful bunions
- Surgical fusion for realignment of bones
- Neuropathy decompression surgery to treat nerve damage
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.