Blogs
Ringworm on the Feet
Ringworm is a type of fungal infection that can affect any part of the body. When it affects the feet, it is also known as athlete’s foot. Athlete’s foot can cause some very unpleasant symptoms, including itching, burning, or stinging between the toes, a red, scaly rash on the feet, dry, flaking, or peeling skin, foot blisters, and a foul odor. The infection can also spread to the toenails causing them to become thickened, brittle, and discolored. Fortunately, fungal infections of the feet tend to respond well to treatment. Your podiatrist may prescribe topical antifungal medications, such as creams or powders, that you apply directly to your feet, or oral antifungal medications that you take by mouth. If you have symptoms of ringworm on your feet, please seek the care of a podiatrist.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with Dr. Dean D. Hinners from Illinois. Our doctor will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
- Thoroughly washing and drying feet
- Avoid going barefoot in locker rooms and public showers
- Using shower shoes in public showers
- Wearing socks that allow the feet to breathe
- Changing socks and shoes frequently if you sweat a lot
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
- Redness
- Burning
- Itching
- Scaly and peeling skin
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How and Where Plantar Warts Occur
When the outer layer of skin on the sole of the feet comes in contact with the human papilloma virus, thickened growths called plantar warts can develop. The virus—which can lurk in public showers, pools, and locker rooms—enters through tiny breaks in the skin on the bottom of feet. These flat, rough masses sometimes have tiny black “dots” in the center, which are actually tiny blood vessels. They can be uncomfortable at times—especially if they occur on weight-bearing areas of the feet and toes. While verrucas can often heal on their own, they can be stubborn, and you may want to see a podiatrist to help get rid of them.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. Dean D. Hinners from Illinois. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What Is Peripheral Artery Disease?
Peripheral artery disease (PAD) causes a narrowing of arteries in the limbs that are not close to the center of the body, such as the legs and feet. These arteries, which carry blood from the heart, become blocked by a buildup of plaque and cannot deliver adequate blood supply to muscles and tissues. This can result in muscle cramping while exercising (claudication) that does not go away after you stop. You may also experience slow-healing foot wounds and slower growth of leg hair and toenails. The skin on your legs may also have a shiny appearance. PAD is potentially dangerous because it increases the risk of a heart attack or stroke. Also, tissue which does not receive enough blood can become infected or die (gangrene) which, left untreated, may lead to a life-threatening blood infection called sepsis. It is important to pay attention and see a podiatrist if your body gives you any warning signs of PAD.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Dr. Dean D. Hinners from Illinois. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What Type of Running Am I Interested In?
 Research has indicated that it may be beneficial to purchase running shoes that are based on the shape of your foot. Additionally, it helps to know what type of running you are planning on doing, as this can aid you in choosing the right style of shoe. Many runners understand the importance of alternating shoes because it helps to prolong the life of the shoes. Feet are typically larger at the end of the day, which is why it’s recommended shoes are tried on at that time. An important quality to look for is a stiff heel, which provides adequate stability for the foot and ankle. If you would like additional information about the qualities to look for in running shoes, it is suggested that you consult with a podiatrist.
Research has indicated that it may be beneficial to purchase running shoes that are based on the shape of your foot. Additionally, it helps to know what type of running you are planning on doing, as this can aid you in choosing the right style of shoe. Many runners understand the importance of alternating shoes because it helps to prolong the life of the shoes. Feet are typically larger at the end of the day, which is why it’s recommended shoes are tried on at that time. An important quality to look for is a stiff heel, which provides adequate stability for the foot and ankle. If you would like additional information about the qualities to look for in running shoes, it is suggested that you consult with a podiatrist.
If you are a runner, wearing the right running shoe is essential. For more information, contact Dr. Dean D. Hinners from Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
To increase performance and avoid the risk of injury, it is important to choose the right running shoe based on your foot type. The general design of running shoes revolves around pronation, which is how the ankle rolls from outside to inside when the foot strikes the ground.
- Neutral runners are able to choose from a wide variety of shoes, including minimalist shoes or even going barefoot.
- Runners who overpronate, or experience an over-abundance of ankle rolling, should choose shoes that provide extra motion control and stability.
- Runners who underpronate, or supinate, have feet that have high arches and lack flexibility, preventing shock absorption. They require shoes with more flexibility and cushion.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What Is Sesamoiditis?
Sesamoid bones are connected to tendons instead of other bones or can be deeply embedded in muscle tissue. The largest sesamoid bone is the kneecap. Two other petite sesamoid bones, the size of corn kernels, are located at the base of the toe in the ball of the foot. When these bones become stressed due to overuse from activities such as ballet dancing, running, playing baseball or similar sports, the tendons surrounding the sesamoid bones become inflamed and painful. This is known as sesamoiditis. Check with a podiatrist if you suspect you are afflicted with sesamoiditis. Sometimes bruising can occur, and if it does it is normally mild. You can cushion the bruise with padding and avoid tight constricting shoes or other sources of friction. Podiatrists can help treat sesamoiditis with icing, compression bandages, and more, while prescribing rest and elevation of the affected foot.
Sesamoiditis is an unpleasant foot condition characterized by pain in the balls of the feet. If you think you’re struggling with sesamoiditis, contact Dr. Dean D. Hinners of Illinois. Our doctor will treat your condition thoroughly and effectively.
Sesamoiditis
Sesamoiditis is a condition of the foot that affects the ball of the foot. It is more common in younger people than it is in older people. It can also occur with people who have begun a new exercise program, since their bodies are adjusting to the new physical regimen. Pain may also be caused by the inflammation of tendons surrounding the bones. It is important to seek treatment in its early stages because if you ignore the pain, this condition can lead to more serious problems such as severe irritation and bone fractures.
Causes of Sesamoiditis
- Sudden increase in activity
- Increase in physically strenuous movement without a proper warm up or build up
- Foot structure: those who have smaller, bonier feet or those with a high arch may be more susceptible
Treatment for sesamoiditis is non-invasive and simple. Doctors may recommend a strict rest period where the patient forgoes most physical activity. This will help give the patient time to heal their feet through limited activity. For serious cases, it is best to speak with your doctor to determine a treatment option that will help your specific needs.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
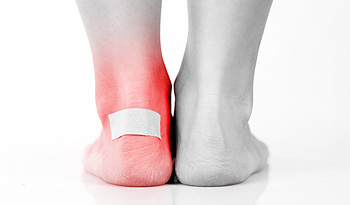
How Exactly Do Blisters Form?
When friction from a shoe or sock rubbing against your skin causes the epidermis (top) layer and dermis (underlying) layer of skin to move in opposite directions, the skin becomes irritated, red, and inflamed. Continued friction will cause the epidermis and dermis to separate and fill with fluid or blood, and a blister is formed. Pain from a blister is caused when nerves are stimulated by the fluid. You can help stop blisters from occurring by wearing shoes that fit properly and don’t allow your feet to slip around or rub against them. New shoes or boots should be worn in properly and gradually—before wearing them all day. If you are planning a long walk or hike, you can try taping areas on the foot that are prone to blisters such as the back of the heel, the big toe and the little toe. A podiatrist can show you how to tape your feet properly and also create custom orthotics designed specifically to keep your feet from developing blisters. They can even suggest appropriate footwear for walking and running.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact Dr. Dean D. Hinners of Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Charcot Marie Tooth Disease and the Feet
Charcot Marie Tooth (CMT) disease is a neurological condition characterized by a weakness and loss of sensation in the legs, hands, and feet due to nerve damage. This condition is genetic, affecting approximately 1 in every 2500 people. CMT develops gradually over time and progressively worsens. While there is no cure, a podiatrist can help you manage the symptoms of CMT in your feet. People with this condition may experience a change in the structure of their feet, developing high arches and hammertoes. Pain, muscle weakness, altered sensation, and muscle cramps are also common. Your podiatrist may recommend a treatment program consisting of foot strengthening and stretching exercises, orthotics, pain medication, and possibly surgery to reduce symptoms and maintain your mobility and quality of life. If you suffer from CMT disease, seeing a podiatrist can help.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with Dr. Dean D. Hinners from Illinois. Our doctor will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
- Numbness
- Sensation loss
- Prickling and tingling sensations
- Throbbing, freezing, burning pains
- Muscle weakness
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What is Tarsal Tunnel Syndrome?
 Tarsal tunnel syndrome is a condition in which the posterior tibial nerve in the tarsal tunnel becomes pinched or compressed. This causes a number of symptoms including burning and shooting pain, a pins and needles sensation, numbness, and tightness in the foot. There are several reasons why the nerve could become compressed, which include bony prominences, bone spurs, abnormal heel position, and the swelling of tendons in the tarsal tunnel. Due to the nature of tarsal tunnel syndrome, diagnosis may be difficult because it can seem to mimic the symptoms of other conditions; heel pain and arch pain are some examples. It is best to see a podiatrist if you are experiencing any of those symptoms. Podiatrists can offer a number of treatments, such as orthotics, taping or bracing, rest, icing, anti-inflammatory medication, or even surgery if other treatments do not improve your condition.
Tarsal tunnel syndrome is a condition in which the posterior tibial nerve in the tarsal tunnel becomes pinched or compressed. This causes a number of symptoms including burning and shooting pain, a pins and needles sensation, numbness, and tightness in the foot. There are several reasons why the nerve could become compressed, which include bony prominences, bone spurs, abnormal heel position, and the swelling of tendons in the tarsal tunnel. Due to the nature of tarsal tunnel syndrome, diagnosis may be difficult because it can seem to mimic the symptoms of other conditions; heel pain and arch pain are some examples. It is best to see a podiatrist if you are experiencing any of those symptoms. Podiatrists can offer a number of treatments, such as orthotics, taping or bracing, rest, icing, anti-inflammatory medication, or even surgery if other treatments do not improve your condition.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Dr. Dean D. Hinners of Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The Elderly and Foot Health
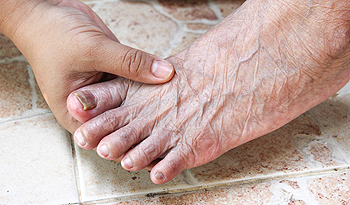 Taking good care of your feet becomes more important as you get older. Age tends to exacerbate foot issues, with many people over the age of 65 reportedly suffering from foot pain. Another common issue among the elderly is diabetes. Diabetes causes neuropathy, or nerve loss, in the lower body, especially in the feet. Diabetics suffer from poor blood circulation in the legs and feet as well. This means that if a diabetic sustains a wound, they may not realize it due to loss of sensation, and the wound may not heal properly. In severe cases, amputation may be necessary if the infection significantly worsens. Because of this, elderly diabetics need to take extra care of their feet, though most elderly people will also benefit from practicing good foot health. Good foot health strategies include daily foot inspections for any abnormalities, washing and drying the feet, keeping one's diabetes in check, and wearing quality socks and footwear that will protect the feet and provide ample foot support. Finally, performing a check-up with a podiatrist yearly is also recommended.
Taking good care of your feet becomes more important as you get older. Age tends to exacerbate foot issues, with many people over the age of 65 reportedly suffering from foot pain. Another common issue among the elderly is diabetes. Diabetes causes neuropathy, or nerve loss, in the lower body, especially in the feet. Diabetics suffer from poor blood circulation in the legs and feet as well. This means that if a diabetic sustains a wound, they may not realize it due to loss of sensation, and the wound may not heal properly. In severe cases, amputation may be necessary if the infection significantly worsens. Because of this, elderly diabetics need to take extra care of their feet, though most elderly people will also benefit from practicing good foot health. Good foot health strategies include daily foot inspections for any abnormalities, washing and drying the feet, keeping one's diabetes in check, and wearing quality socks and footwear that will protect the feet and provide ample foot support. Finally, performing a check-up with a podiatrist yearly is also recommended.
Proper foot care is something many older adults forget to consider. If you have any concerns about your feet and ankles, contact Dr. Dean D. Hinners from Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
The Elderly and Their Feet
As we age we start to notice many changes in our body, but the elder population may not notice them right away. Medical conditions may prevent the elderly to take notice of their foot health right away. Poor vision is a lead contributor to not taking action for the elderly.
Common Conditions
- Neuropathy – can reduce feeling in the feet and can hide many life-threatening medical conditions.
- Reduced flexibility – prevents the ability of proper toenail trimming, and foot cleaning. If left untreated, it may lead to further medical issues.
- Foot sores – amongst the older population can be serious before they are discovered. Some of the problematic conditions they may face are:
- Gouging toenails affecting nearby toe
- Shoes that don’t fit properly
- Pressure sores
- Loss of circulation in legs & feet
- Edema & swelling of feet and ankles
Susceptible Infections
Diabetes and poor circulation can cause general loss of sensitivity over the years, turning a simple cut into a serious issue.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Causes of Heel Spurs
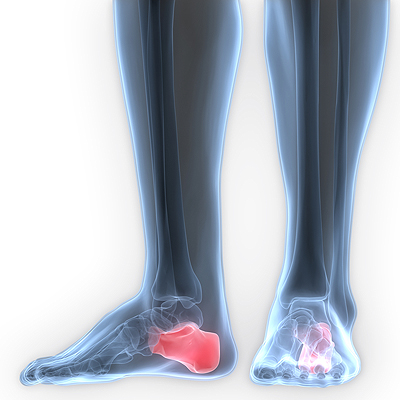 If a tiny bone protrudes from the heel of the foot, you may have what is known as a heel spur. This condition occurs when the portion of tissue that connects the heel to the toes sustains an injury. Early symptoms may consist of swelling, pain, and general discomfort, and these typically occur while walking. Other contributing reasons for this condition can include weight gain or if the wrong shoes are worn. To properly diagnose this condition, an X-ray is typically performed to view the bone protrusion. There are several treatment options available, and these may include properly stretching the calf muscles, losing excess weight, and wearing shoes that fit correctly. It’s advised to schedule a consultation with a podiatrist to receive a proper diagnosis and to learn about the best treatment options for your heel spur.
If a tiny bone protrudes from the heel of the foot, you may have what is known as a heel spur. This condition occurs when the portion of tissue that connects the heel to the toes sustains an injury. Early symptoms may consist of swelling, pain, and general discomfort, and these typically occur while walking. Other contributing reasons for this condition can include weight gain or if the wrong shoes are worn. To properly diagnose this condition, an X-ray is typically performed to view the bone protrusion. There are several treatment options available, and these may include properly stretching the calf muscles, losing excess weight, and wearing shoes that fit correctly. It’s advised to schedule a consultation with a podiatrist to receive a proper diagnosis and to learn about the best treatment options for your heel spur.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact Dr. Dean D. Hinners from Illinois. Our doctor will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the latest in diagnostic and treatment technology to meet your needs.
More...
Common Symptoms of Sesamoiditis
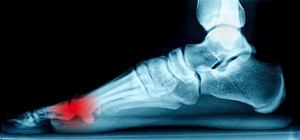 If you experience pain under the ball of your foot, you may have a condition that is referred to as sesamoiditis. There are small bones that exist within the sole of the foot, and a possible injury can cause inflammation to the tendons that connect the big toe to these bones. If this should happen, common symptoms may include pain being present while walking and running, in addition to experiencing difficulty standing on tiptoes. The skin typically does not show any signs of being swollen or red because the injured bones and tendons are deep within the foot. It generally stems from beginning any new activity that may involve running and jumping, typically indicative of a new sport. If you feel you are suffering from this ailment, it’s suggested that resting the foot by reducing the activity will be beneficial in promoting healing. Please consider a consultation with a podiatrist for more information about sesamoiditis.
If you experience pain under the ball of your foot, you may have a condition that is referred to as sesamoiditis. There are small bones that exist within the sole of the foot, and a possible injury can cause inflammation to the tendons that connect the big toe to these bones. If this should happen, common symptoms may include pain being present while walking and running, in addition to experiencing difficulty standing on tiptoes. The skin typically does not show any signs of being swollen or red because the injured bones and tendons are deep within the foot. It generally stems from beginning any new activity that may involve running and jumping, typically indicative of a new sport. If you feel you are suffering from this ailment, it’s suggested that resting the foot by reducing the activity will be beneficial in promoting healing. Please consider a consultation with a podiatrist for more information about sesamoiditis.
Sesamoiditis is an unpleasant foot condition characterized by pain in the balls of the feet. If you think you’re struggling with sesamoiditis, contact Dr. Dean D. Hinners of Illinois. Our doctor will treat your condition thoroughly and effectively.
Sesamoiditis
Sesamoiditis is a condition of the foot that affects the ball of the foot. It is more common in younger people than it is in older people. It can also occur with people who have begun a new exercise program, since their bodies are adjusting to the new physical regimen. Pain may also be caused by the inflammation of tendons surrounding the bones. It is important to seek treatment in its early stages because if you ignore the pain, this condition can lead to more serious problems such as severe irritation and bone fractures.
Causes of Sesamoiditis
- Sudden increase in activity
- Increase in physically strenuous movement without a proper warm up or build up
- Foot structure: those who have smaller, bonier feet or those with a high arch may be more susceptible
Treatment for sesamoiditis is non-invasive and simple. Doctors may recommend a strict rest period where the patient forgoes most physical activity. This will help give the patient time to heal their feet through limited activity. For serious cases, it is best to speak with your doctor to determine a treatment option that will help your specific needs.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Why is it Important for Seniors to Maintain Proper Foot Care?
 There are several ways seniors can practice proper foot care. These may include wearing shoes that fit correctly and are comfortable to wear during daily activities. It’s important the toes have adequate room to move around inside, and this may possibly avoid a pre-existing case of bunions from becoming worse. It may also prevent corns from developing. Additionally, performing a gentle exercise program frequently, may aid in keeping the blood flowing. These may include walking and stretching, which may help to maintain proper circulation. Washing the feet and drying thoroughly between the toes may be beneficial in preventing athlete’s foot from developing. When a moisturizing lotion is used, a painful condition referred to as cracked heels may be avoided. When the toenails are trimmed properly, occurrences of ingrown toenails may decrease. If you are a senior, it’s suggested to consult with a podiatrist on a frequent basis to discuss any foot conditions that may be present.
There are several ways seniors can practice proper foot care. These may include wearing shoes that fit correctly and are comfortable to wear during daily activities. It’s important the toes have adequate room to move around inside, and this may possibly avoid a pre-existing case of bunions from becoming worse. It may also prevent corns from developing. Additionally, performing a gentle exercise program frequently, may aid in keeping the blood flowing. These may include walking and stretching, which may help to maintain proper circulation. Washing the feet and drying thoroughly between the toes may be beneficial in preventing athlete’s foot from developing. When a moisturizing lotion is used, a painful condition referred to as cracked heels may be avoided. When the toenails are trimmed properly, occurrences of ingrown toenails may decrease. If you are a senior, it’s suggested to consult with a podiatrist on a frequent basis to discuss any foot conditions that may be present.
Proper foot care is something many older adults forget to consider. If you have any concerns about your feet and ankles, contact Dr. Dean D. Hinners from Illinois. Our doctor can provide the care you need to keep you pain-free and on your feet.
The Elderly and Their Feet
As we age we start to notice many changes in our body, but the elder population may not notice them right away. Medical conditions may prevent the elderly to take notice of their foot health right away. Poor vision is a lead contributor to not taking action for the elderly.
Common Conditions
- Neuropathy – can reduce feeling in the feet and can hide many life-threatening medical conditions.
- Reduced flexibility – prevents the ability of proper toenail trimming, and foot cleaning. If left untreated, it may lead to further medical issues.
- Foot sores – amongst the older population can be serious before they are discovered. Some of the problematic conditions they may face are:
- Gouging toenails affecting nearby toe
- Shoes that don’t fit properly
- Pressure sores
- Loss of circulation in legs & feet
- Edema & swelling of feet and ankles
Susceptible Infections
Diabetes and poor circulation can cause general loss of sensitivity over the years, turning a simple cut into a serious issue.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How Many Different Types of Corns Are There?
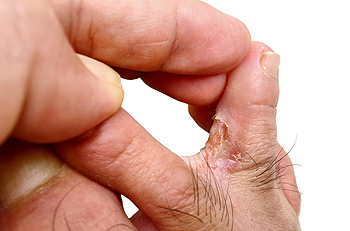 If you have ever experienced a corn on the top of the toes, you most likely are aware of the pain that is associated with it. Corns are generally the result of increased pressure and rubbing, and typically originates from shoes that do not fit correctly. It appears to be a small area, and the skin will be hardened and thick. There are known to be two types of corns and are referred to as hard and soft corns. The latter generally develops in between the toes and are often soft, because of the excess moisture and sweat that is present. Hard corns come from wearing shoes that are too tight and may often cause the toes to endure unwanted pressure, resulting in pain and discomfort. There are different types of treatments that may be used to eliminate corns, and it’s advised to speak with a podiatrist for possible relief options that are correct for you.
If you have ever experienced a corn on the top of the toes, you most likely are aware of the pain that is associated with it. Corns are generally the result of increased pressure and rubbing, and typically originates from shoes that do not fit correctly. It appears to be a small area, and the skin will be hardened and thick. There are known to be two types of corns and are referred to as hard and soft corns. The latter generally develops in between the toes and are often soft, because of the excess moisture and sweat that is present. Hard corns come from wearing shoes that are too tight and may often cause the toes to endure unwanted pressure, resulting in pain and discomfort. There are different types of treatments that may be used to eliminate corns, and it’s advised to speak with a podiatrist for possible relief options that are correct for you.
Corns can make walking very painful and should be treated immediately. If you have questions regarding your feet and ankles, contact Dr. Dean D. Hinners of Illinois. Our doctor will treat your foot and ankle needs.
Corns: What Are They? And How Do You Get Rid of Them?
Corns are thickened areas on the skin that can become painful. They are caused by excessive pressure and friction on the skin. Corns press into the deeper layers of the skin and are usually round in shape.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as:
- Wearing properly fitting shoes that have been measured by a professional
- Wearing shoes that are not sharply pointed or have high heels
- Wearing only shoes that offer support
Treating Corns
Although most corns slowly disappear when the friction or pressure stops, this isn’t always the case. Consult with your podiatrist to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Wearing Flip Flops May Negatively Affect The Feet
 Research has indicated that frequently wearing flip flops may cause unpleasant foot conditions to gradually develop. These can include heel and ankle pain, in addition to increasing the likelihood of stubbing your toe, which may lead to a broken toe. The average flip flop has minimal support for the overall foot. This includes little cushioning in the heel and arch area, which can contribute to a lack of shock absorption. The toes may undergo stress as they attempt to keep the shoe on the foot, as a result of excessive gripping. People who wear this type of shoe often take shorter steps, which may alter their style of walking. Painful conditions such as heel spurs and plantar fasciitis may develop as a result of wearing flip flops. Additional information is available from a podiatrist about the harmful effects wearing flip flops could have on the feet.
Research has indicated that frequently wearing flip flops may cause unpleasant foot conditions to gradually develop. These can include heel and ankle pain, in addition to increasing the likelihood of stubbing your toe, which may lead to a broken toe. The average flip flop has minimal support for the overall foot. This includes little cushioning in the heel and arch area, which can contribute to a lack of shock absorption. The toes may undergo stress as they attempt to keep the shoe on the foot, as a result of excessive gripping. People who wear this type of shoe often take shorter steps, which may alter their style of walking. Painful conditions such as heel spurs and plantar fasciitis may develop as a result of wearing flip flops. Additional information is available from a podiatrist about the harmful effects wearing flip flops could have on the feet.
Flip-flops can cause a lot of problems for your feet. If you have any concerns about your feet or ankles, contact Dr. Dean D. Hinners from Illinois. Our doctor will assist you with all of your foot and ankle needs.
Flip-Flops and Feet
Flip-flops have managed to become a summer essential for a lot of people. While the shoes may be stylish and easy to slip on and off, they can be dangerous to those who wear them too often. These shoes might protect you from fungal infections such as athlete’s foot, but they can also give you foot pain and sprained ankles if you trip while wearing them.
When Are They Okay to Wear?
Flip-flops should only be worn for very short periods of time. They can help protect your feet in places that are crawling with fungi, such as gym locker rooms. Athlete’s foot and plantar warts are two common fungi that flip-flops may help protect your feet against.
Why Are They Bad for My Feet?
These shoes do not offer any arch support, so they are not ideal for everyday use. They also do not provide shock absorption or heel cushioning which can be problematic for your feet. Additionally, you may suffer from glass cuts, puncture wounds, and stubbed toes since they offer little protection for your feet.
More Reasons Why They Are Bad for Your Feet
- They Slow You Down
- May Cause Blisters and Calluses
- Expose Your Feet to Bacteria
If you have any questions, please feel free to contact one of our offices located in Metropolis and Eldorado, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.